Research
We have a bold ambition: to stop prostate cancer limiting men's lives. And it’s through funding research that we will make this happen.

TRANSFORM trial
Discover our biggest and most ambitious trial ever, designed to find the best way to screen for prostate cancer.
TRANSFORM trial
Our research strategy
Our research strategy sets out how we will invest to improve the lives of men with prostate cancer
Our research strategy
Research we fund
We fund innovative and ground-breaking projects thanks to your support
Research we fund

The impact of our research
Our pioneering research is paving the way to a better future for men with prostate cancer
Research impact

Latest news

Introducing TRANSFORM, our £42 million trial to find a screening programme for prostate cancer
The £42 million TRANSFORM trial, our biggest and most ambitious trial ever, could save the lives of thousands of men each year.
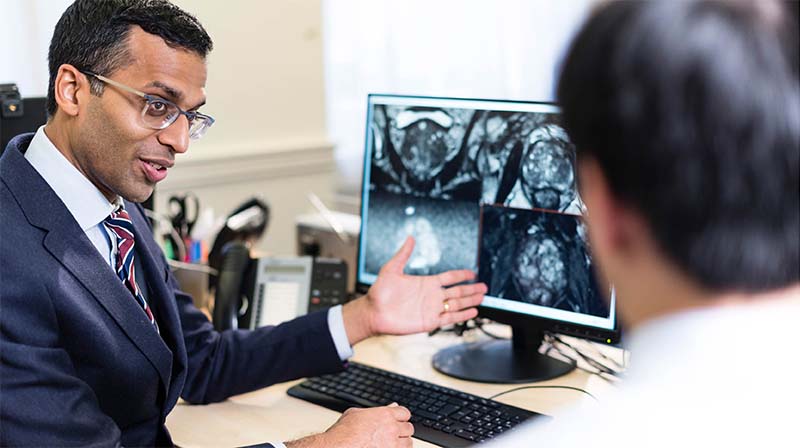
Simple changes can vastly increase MRI quality, giving men a faster, more accurate diagnosis
The changes could benefit huge numbers of men worldwide, preventing thousands of biopsies and making others more accurate.

Blocking ‘SOS’ signals from prostate cancer cells key to stopping treatment resistance
Prostate Cancer UK-funded researchers have discovered how prostate cancer cells harness the immune system to resist treatments. The finding could lead to new, more effective ways to treat advanced prostate cancer.

Can we manipulate sugar molecules and gut bugs to treat prostate cancer?
We've just invested a huge £3m into revolutionary research as we hunt for the next generation of tests and treatments.
